Upper Cross Syndrome: Today’s most common posture
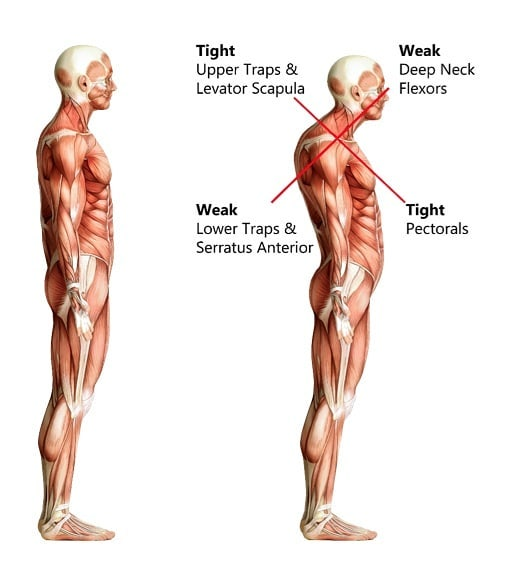
Upper cross syndrome is a term used to describe a distorted posture. For example, imagine an individual whose shoulders are slumped and whose head and neck jut forward. It is the most common posture in today’s society. This forward head posture is linked to our lifestyles. After all, our lives revolve around our smart phones and desk jobs.
Upper cross Syndrome is a chronic shortening of the sub-occipital muscles. This leads to headaches, as well as head and neck pain.
However, there is a technique that can be very effective for those developing upper cross syndrome.
This technique is known as Sub-Occipital Release technique. This release is used to stretch and soften these muscles to improve pain and posture. Also, it releases the fascia and muscles surrounding and supporting the head and neck.
The Sub-Occipital Release is an Osteopathic technique.
The best part – it’s simple, safe and very effective.
The Sub-Occipital Release helps to soften the fascia and muscle tissue in the sub-occipital area. This helps to open up the area between the C1 (Atlas) and C2 (Axis) vertebrae. These vertebrae are at the top of the neck and the base of the head. This is also known as the occiput.
The Sub-Occipital Release is also used in the treatment of tension headaches, neck pain, shoulder pain and upper back pain.
To experience the benefits of sub-occipital release with Deepak, our Osteopath,
click the button below.